Phone
866-411-EARS
Address
PhotoniCare Inc.
2800 Meridian Parkway, Suite 175
Durham, NC 27713
Everyone remembers having ear infections. As a child, it was probably one of the more frustrating things to endure. Your ear hurt and your hearing was muffled. Thankfully, as we grow older, ear infections become less common (although they do happen) but they are frequently present during childhood.
Something most people don’t know is that there are actually two different types of ear infections. Most just assume that there is just one type and it’s the painful kind you remember; however, there is Acute Otitis Media and Otitis Media with Effusion. Don’t know how each one affects you? You’re not alone, and we’re here to help.
Acute Otitis Media
Acute Otitis Media (or AOM) is an ear infection where the middle ear (area behind the eardrum) becomes inflamed and infected. The eustachian tube that runs from the middle of the ear to the back of the throat becomes swollen, trapping infected fluid in the middle ear. This occurs due to a variety of reasons including the flu and common cold. Because the eustachian tube is much shorter and more horizontal in children, it can become blocked much easier than in adults, and is more susceptible to middle ear infection. Since this happens to young children, sometimes it can be tough for them to explain exactly how they are feeling, so parents have to be extra vigilant when it comes to looking for symptoms. Some things parents can look for are the following:
When one of these symptoms is present, it may be time to get the child to their healthcare provider. When a provider checks you or your child for an ear infection, they will typically use an instrument called an otoscope. An otoscope is basically a pen light attached to a magnifying glass, and this simple device has been used in medicine for the past 150 years. The otoscope comes with several cone-like tips called specula. The healthcare provider will gently insert the speculum into the ear canal to try to get a view of the surface of the eardrum. While the otoscope view of the eardrum may provide some relevant information, such as an inflamed and/or bulging eardrum, it cannot view the middle ear where the infection actually resides.
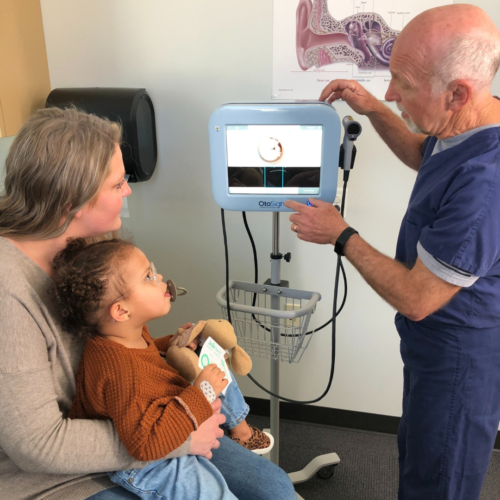
Future technologies, such as the OtoSight Middle Ear Scope, will allow clinicians to view the middle ear by seeing through the eardrum. If the healthcare provider does suspect an ear infection, antibiotics may or may not be recommended. Generally speaking, an ear infection has the potential to resolve itself without antibiotic treatment. In the case of a severe middle ear infection with infected fluid in the middle ear, the American Academy of Pediatrics recommends the healthcare provider prescribe antibiotics. And in cases where multiple ear infections have occurred, called Recurrent AOM (RAOM), a referral to an ear specialist (otolaryngologist) may be necessary, to evaluate whether surgical intervention may be warranted. However, the guidelines recommend a “watchful waiting” approach for non-severe middle ear infections in children over the age of two. The overall goal is to reduce over-prescription of antibiotics.
Otitis Media with Effusion
Otitis Media with Effusion (OME) occurs when the eustachian tube clogs and fluid cannot drain from your ears to the back of your throat. It is incredibly common and, according to the Agency of Healthcare Research and Quality, around 90% of children will have OME by the time they turn ten. Just like with AOM, children are much more likely to get OME because of their shorter and more horizontal eustachian tubes. Also, children contract more colds and other viral upper respiratory illnesses with more regularity than adults. While OME is not actually an ear infection, they are closely related. By developing OME, the middle ear fluid serves as a breeding ground for bacteria to grow, which may lead to AOM.
One of the major symptoms of OME is hearing problems. You may notice your child turning the television up louder, having to ask you to repeat yourself more or saying things sound muffled. He or she may also be continuously tugging at the ear. If you have a suspicion that your child has OME, you can take him or her to the doctor where further testing can be done. Similar to AOM diagnosis, a doctor can use an otoscope or conduct a tympanometry test to see if the child does in fact have OME. However, current tools used to diagnose fluid in the middle ear can be difficult to use reliably in squirming or crying children, and rely heavily on user expertise to interpret a simple image or measurement of the eardrum, especially in primary care settings where otoscopic accuracy has been reported to be as low as 50%. If your child is diagnosed with OME, it can usually be cleared up by just giving it time.
A complication that can arise when fluid stays in the ear for an extended period of time (3 months or more) or comes back time and again is Chronic OME (COME). When a person develops COME, he or she can find it harder to fight off future ear infections and his or her hearing may be permanently affected. If it happens in children it may have an impact on speech development. Referral to an otolarygologist for suspected COME may require surgical intervention to drain the fluid and air out the middle ear.
Again, OME is incredibly common and may not have any long-term effect on a child’s health as long as it does not become a chronic issue. Washing hands regularly, avoiding allergens, utilizing air filters and avoiding cigarette smoke and air pollution are just a few ways to avoid contracting OME.

The COVID-19 pandemic has created numerous challenges for parents. Navigating… Read More
PhotoniCare sits down with Dr. Michael Novak, an Ear, Nose… Read More

This week on the #EnginEarGuys blog we talk about otolaryngology… Read More